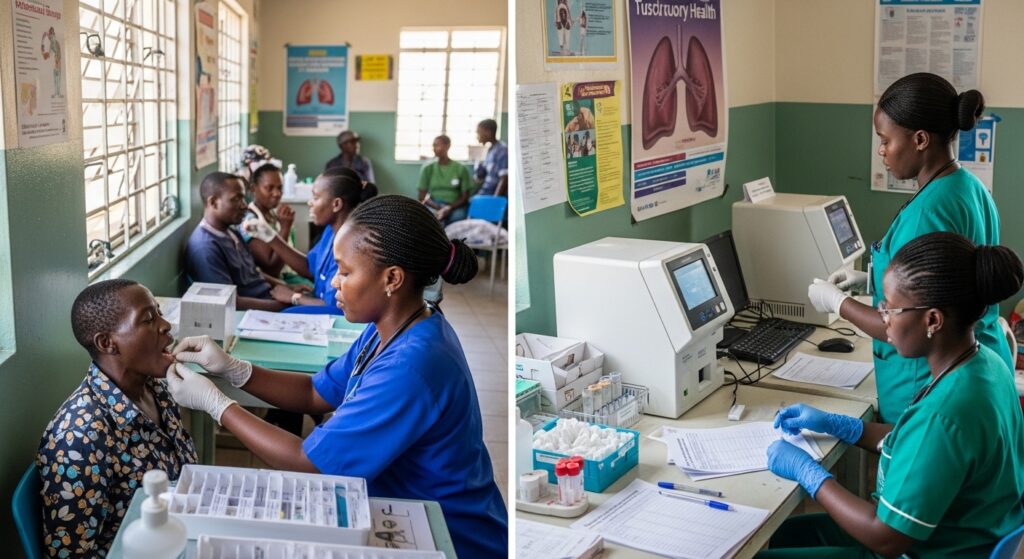
New World Health Organization recommendations are widening the front line of tuberculosis detection, backing simpler molecular tests near the point of care and endorsing tongue-swab sampling for some patients in a move aimed at finding cases earlier and getting lifesaving treatment started sooner.
The change may sound technical, but its implications are practical and urgent. Tuberculosis remains one of the world’s deadliest infectious diseases, and one of the biggest barriers to controlling it is that too many people are still diagnosed late, diagnosed with slower tools, or not diagnosed at all. By pushing testing closer to where patients first seek care — and by supporting sample collection methods that are easier than traditional sputum-based diagnosis in some circumstances — WHO is trying to narrow one of the most stubborn gaps in the global TB response.
In guidance highlighted around World TB Day this year, WHO urged countries to accelerate the uptake of new diagnostic tools, including tests that can be used near the point of care and tongue swabs that can help detect disease faster and reach more people. The organization also linked the diagnostic push directly to expanded access to treatment, reflecting a central truth in TB control: people cannot benefit from modern medicines if health systems fail to find them in time.
The new recommendations build on a basic problem that TB programs have struggled with for years. Standard sputum collection can be difficult, especially for people who are very ill, frail, or simply unable to produce a good respiratory sample when asked. That challenge is not minor. In the real world, every failed sample can become a missed diagnosis, a delayed diagnosis, or an additional clinic visit that a poor or remote patient may never complete. WHO’s updated policy therefore matters not only because it endorses new laboratory approaches, but because it acknowledges the lived logistics of diagnosis.
Near-point-of-care molecular tests sit at the center of that shift. These are designed to be used closer to patients than more centralized laboratory platforms, while still delivering the kind of rapid nucleic-acid-based detection that has increasingly replaced older smear microscopy as the preferred standard. WHO now recommends near-point-of-care nucleic acid amplification tests on sputum as initial diagnostic tests for adults and adolescents with signs and symptoms of pulmonary TB, or who screen positive for it, rather than relying on smear microscopy. The aim is straightforward: reduce the time and complexity between suspicion of disease and a reliable answer.
The more novel and attention-grabbing change is WHO’s support for tongue swabs in selected circumstances. In updated guidance, the organization says that when sputum cannot be obtained, near-point-of-care molecular tests on tongue swabs should be used as initial diagnostic tests for TB. WHO has also updated recommendations on low-complexity automated molecular tests to include tongue swabs for the initial detection of pulmonary TB among adults and adolescents who screen positive and cannot produce sputum. This is significant because it opens a new diagnostic pathway for people who might otherwise be left outside the testing system altogether.
Tongue swabs are appealing for obvious reasons. They are easier to collect, less invasive, and simpler to handle than sputum in many frontline settings. They may also be particularly useful in decentralized care models, where health workers need sample-collection methods that are quick, acceptable and feasible in busy clinics or lower-resource environments. For patients, that can mean less discomfort and fewer practical barriers. For health systems, it can mean a better chance of converting a suspected case into an actual test on the first visit.
WHO is not presenting the shift as a miracle cure or a replacement for all existing TB diagnostics. The organization’s language is more careful than that. What it is doing is expanding the toolkit. In addition to near-point-of-care tests and tongue swabs, WHO is also recommending sputum pooling as a cost-saving strategy to increase testing efficiency for TB and rifampicin-resistant TB. The broader message is that diagnostic systems need to become more flexible, more accessible and more efficient if countries are to close the detection gap at scale.
That gap remains alarmingly large. According to WHO’s Global Tuberculosis Report 2025, an estimated 10.7 million people fell ill with TB in 2024, while only 8.3 million were reported as newly diagnosed, equivalent to 78% of the estimated total. The shortfall means about 2.4 million people were either not diagnosed or not officially reported to national authorities. Those are not just statistical absences. They represent untreated disease, avoidable deaths, continued household transmission and opportunities lost.
WHO’s own framing makes clear that faster diagnosis is inseparable from survival. The organization said more than 1.2 million people died from TB in 2024, even though the disease is preventable and curable. It also emphasized that treatment of people with TB is estimated to have averted 83 million deaths from 2000 to 2024. Those figures explain why diagnostic policy is not merely a laboratory issue. Earlier detection can change whether someone receives treatment before becoming critically ill, whether drug resistance is recognized in time, and whether transmission continues in homes and communities.
The recommendation also reflects a larger strategic change in global health delivery: decentralization. For years, many health systems have depended too heavily on centralized diagnostic infrastructure that works on paper but can fail patients in remote, under-resourced or overloaded settings. Near-point-of-care testing addresses that bottleneck by moving rapid diagnostics closer to community clinics and lower-level facilities. It is an attempt to reorganize TB care around the patient’s pathway rather than around the convenience of the system.
That matters especially in high-burden countries, where distance, transport costs, repeat visits and laboratory turnaround times can all undermine care. A person who must return multiple times for sample collection, testing and result confirmation is a person at high risk of dropping out of the process. By simplifying both the test pathway and the specimen pathway, WHO is effectively trying to reduce attrition before treatment even begins.
Still, recommendations alone do not diagnose anyone. The success of the new policy will depend on implementation: procurement, training, quality assurance, biosafety, program readiness and financing. WHO has acknowledged that reality by pairing the guidance with an implementation toolkit for near-point-of-care and swab-based TB testing, intended to help countries plan rollout, assess readiness, train staff and monitor performance. That is a sign that the organization understands the difference between announcing innovation and making it operational.
There are also scientific and programmatic limits that will need careful handling. Tongue-swab testing is being recommended in defined situations, not as a blanket substitute for all respiratory sampling. Countries will need to integrate the new tools into existing algorithms without creating confusion about when to use which sample and which platform. As with many diagnostic advances, the promise lies not only in the test itself but in disciplined use.
Even so, the direction of travel is unmistakable. WHO is signaling that TB diagnosis must become faster, more decentralized and more adaptable to the real conditions under which patients live and health workers operate. In that sense, the recommendation is about more than technology. It is about access.
For decades, TB control has suffered from a cruel mismatch: the disease is curable, but the path to diagnosis is too often slow, fragile or out of reach. Near-point-of-care testing and tongue swabs will not solve every weakness in the system. But by making it easier to test earlier and in more places, they may help move diagnosis closer to where it has always needed to be — in front of the patient, not beyond reach.