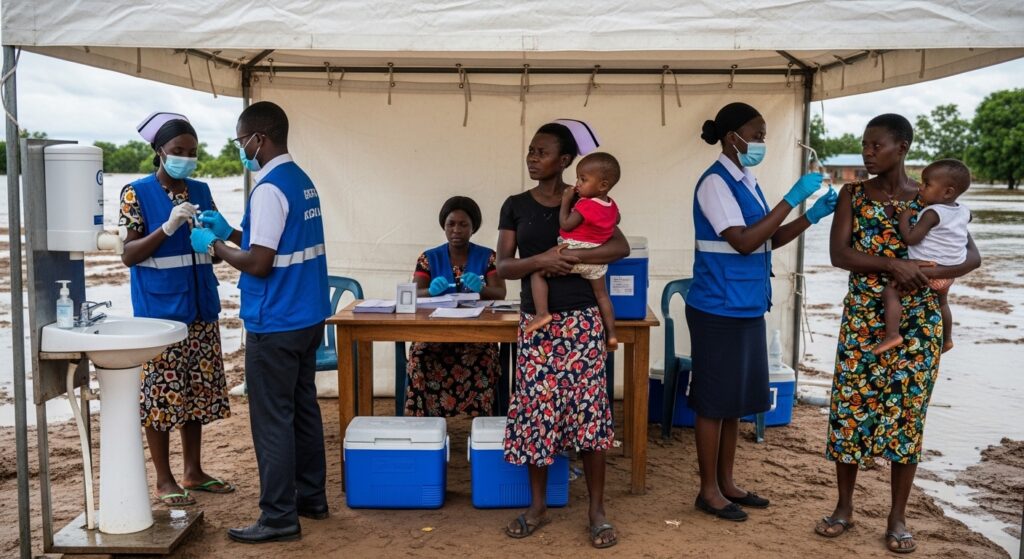
With oral cholera vaccine supply recovering after a prolonged global shortage, health agencies say the shift marks a crucial move from constant emergency response back toward prevention, though major risks from outbreaks, poor sanitation and climate shocks remain.
GENEVA — The World Health Organization, Gavi and UNICEF say the world has reached a turning point in the fight against cholera: after more than three years of disruption to preventive oral cholera vaccination campaigns — a pause that began in 2022 and stretched across nearly four calendar years — global supply has recovered enough to restart mass prevention efforts in vulnerable countries.
The announcement marks a significant change in strategy for a disease that has surged across multiple regions since 2021, overwhelming fragile health systems and forcing global health agencies into a defensive posture. During the shortage, vaccine doses from the global stockpile were largely reserved for urgent outbreak response, with authorities often forced to prioritize reactive campaigns in countries already facing cholera transmission rather than broader preventive drives meant to stop outbreaks before they begin.
Now, WHO and its partners say that balance can begin to shift.
In a joint announcement issued on February 4, the agencies said global oral cholera vaccine supply had risen to a level sufficient to allow the resumption of “life-saving preventive campaigns” for the first time in over three years. Mozambique became the first country to restart preventive vaccination, with further campaigns planned in Bangladesh and the Democratic Republic of the Congo.
The change is more than symbolic. For much of the past several years, the international cholera response has been shaped by scarcity. Health agencies had to decide where limited doses could do the most immediate good as outbreaks multiplied and demand far outstripped supply. That pressure led in October 2022 to a temporary shift away from the standard two-dose approach in emergency settings toward a one-dose strategy, a measure designed to stretch the stockpile further during an acute global shortage.
The shortage reflected a collision of forces. Cholera cases rose sharply around the world, fueled by conflict, displacement, climate-related disasters, weak water and sanitation systems, and rising humanitarian need. WHO said 473,000 cholera cases were reported in 2022, more than double the number in 2021. Preliminary data for 2023 showed the number climbing again to more than 700,000. At the same time, vaccine manufacturing capacity lagged behind the abrupt surge in requests from countries trying to contain outbreaks.
By early 2024, the gap had become severe. WHO reported that from January 2023 to February 2024, countries requested 79 million doses from the stockpile, roughly double the 40 million doses available during that period. In practice, that meant cholera vaccination policy was no longer being driven primarily by optimal public health planning, but by the harsh arithmetic of shortage.
The reopening of preventive campaigns became possible because supply finally began to catch up. WHO said annual global oral cholera vaccine supply doubled from 35 million doses in 2022 to nearly 70 million doses in 2025. A major part of that recovery came from expanded production by EuBiologics, currently the only manufacturer supplying cholera vaccines at the scale needed for global mass campaigns. In 2024, WHO partners also welcomed the prequalification of Euvichol-S, a simplified oral cholera vaccine formulation expected to boost manufacturing volumes, reduce production complexity and lower costs.
The resumption is being backed by a first allocation of 20 million doses for preventive campaigns. Of those, WHO said 3.6 million doses were delivered to Mozambique, 6.1 million to the Democratic Republic of the Congo, and 10.3 million were planned for Bangladesh. The doses are financed by Gavi and procured and delivered by UNICEF.
For global health officials, the decision is an attempt to break what WHO Director-General Tedros Adhanom Ghebreyesus described as a damaging cycle of reaction rather than prevention. In the years of shortage, agencies repeatedly found themselves sending vaccines only after cholera had already spread. Preventive campaigns had effectively been crowded out by emergency firefighting.
That distinction matters because cholera is both preventable and treatable, yet it remains capable of killing quickly in places where clean water, sanitation, hygiene services and timely treatment are not available. The disease spreads through contaminated food and water and can trigger severe diarrhea and dehydration. In the poorest and most crisis-affected settings, even a controllable disease can turn lethal with alarming speed.
Mozambique illustrates why the return of preventive vaccination is being treated as a milestone. WHO said the country launched the first preventive campaign while still dealing with an ongoing outbreak and the aftermath of flooding that affected more than 700,000 people and displaced many others. Floods damaged water systems and disrupted health services, increasing the risk of waterborne disease. In such settings, waiting for an outbreak to intensify before sending vaccine can cost critical time.
The same logic applies to Bangladesh and the Democratic Republic of the Congo, both of which face recurrent cholera risk under conditions shaped by population pressure, fragile sanitation systems or active outbreaks. WHO said the countries selected for the first preventive allocations were chosen under criteria set by the Global Task Force for Cholera Control, a partnership of more than 50 organizations aimed at ensuring the stockpile is used in a systematic, equitable and transparent way.
Still, the agencies are also warning against any impression that the vaccine supply problem is permanently solved. Cholera remains a disease of inequality, infrastructure failure and repeated crisis. Vaccination can reduce risk and buy time, but it cannot substitute for safe drinking water, functioning sewage systems, hygiene access and resilient health services.
UNICEF Executive Director Catherine Russell said the increase in doses would, for the first time in years, allow agencies to better prevent large-scale cholera emergencies, especially for children. But she also stressed that vaccination must go hand in hand with better access to safe water and sanitation. That message echoes years of WHO guidance that oral cholera vaccines are an important tool, but only one element of a broader control strategy.
That broader strategy has become harder to sustain in an era of climate shocks and overlapping crises. WHO has linked the rise in cholera to climate-related extremes, economic insecurity, conflict and population displacement — all factors that weaken water and sanitation systems and make outbreaks harder to contain. In other words, the vaccination recovery is arriving just as the structural drivers of cholera remain dangerously intact.
For Gavi, which finances the stockpile and campaign delivery, the announcement also carries an industrial and market message. Vaccine supply for neglected diseases cannot be treated as an afterthought if the world expects to respond effectively to outbreaks. Gavi CEO Sania Nishtar said the recent surge in cases and unprecedented demand showed that sustainable and accessible vaccine supply is a global public good. Her warning was blunt: the world cannot afford complacency.
That concern is especially relevant because the current recovery still depends heavily on a narrow manufacturing base. EuBiologics remains the central supplier to the global stockpile, leaving global preparedness vulnerable if production falters or demand spikes again. WHO and its partners have openly urged more manufacturers to enter the market, both to strengthen supply security and to reduce the risk of future disruptions.
The return of preventive vaccination, then, is both a breakthrough and a reminder of fragility. It suggests the global system can recover from an emergency stretch in which it was constantly forced to ration protection. But it also exposes how easily vaccine access can collapse when disease outbreaks outpace production.
For countries on the front line, the practical impact may be immediate. Preventive campaigns can help protect communities before seasonal surges, flooding or displacement turn latent risk into active transmission. They may also relieve pressure on emergency health responses that have been forced to chase one outbreak after another. In the best case, they allow public health authorities to act earlier, more strategically and with fewer impossible trade-offs.
Yet the success of this new phase will be judged not by the announcement itself, but by whether it helps reduce outbreaks in places where cholera has become a recurring marker of state fragility and humanitarian neglect. Vaccines can blunt the threat, but they cannot by themselves fix the underlying conditions that let cholera spread.
After years in which the global response was shaped by shortage and triage, WHO and its partners are trying to restore a more proactive model. The resumption of preventive oral cholera vaccination is a major milestone in that effort. But it is also a test — of supply chains, political will, donor commitment and whether the world can move beyond reacting to cholera only when it is already too late.